Family-Full, We Are by Modern Fertility Treatments as PGD in India
Words do nothing Remedial until they recuperate you Healthier
Today, the science of healthy living has its chapter mentioned at everyone’s regular activities. Yes, the healthy living we all ought to live with is thoroughly none other than Tonic to accentuate your smiles. Not only do people from overseas are likely to be found living around the modern medical solutions, but also laity of India to have been inhaling derivations of modern living.
So relying on the most excellent remedial addresses takes in best for the healthy living. Even the infertility issues become wrinkles of infertile parents for a long time has found today answer to their question. In India, there are various addresses to believe on, but do not bring out their services relevant to people’s interest. At us, get thoroughly an abundance of fertility treatments in India (IVF, Surrogacy and more).
Key features of WORLD FERTILITY SERVICES
- Highly top-notch technologies and advanced methods
- Top consultation and counseling session
- Highly experienced fertility and IVF doctor in India
- Affordable IVF treatment with various packages
- Highest success rates of IVF in India
- Contact us: possible@worldfertilityservices.com
- Call us: +91-9560712022

Though IVF PGD in India is often used to refer to any testing performed on an embryo prior to it being transferred to the uterus, Pre-implantation genetic screening could assess the status of an embryo with regard to its chromosomal composition.
Though our Pre-Implantation Genetic Diagnosis (PGD), PGD in India renders as the process of removing a cell from an in vitro fertilization embryo for genetic testing before moving the embryo to the uterus, Pre-Implantation Genetic Screening (PGS) is accomplished as part of in vitro fertilization (IVF) process used to treat infertile couples.
Difference between PGD and PGS
For those who fall with a known genetic abnormality, such as a single gene defect, they undergo Pre-Implantation Genetic Diagnosis. Those for whom this technology is a tool to assist screen embryos for an irregular number of chromosomes are supposed to be having screening performed, therefore the use of term Pre-Implantation Genetic Screening.
About:
WORLD FERTILITY SERVICES is present to help every couple. You can have the best infertility treatment with top guidance. Moreover, the best IVF centre in India has advanced technologies and techniques for various treatments. Many patients choose us for their successful procedures and outcome. With it, you can have detailed IVF cost in India. It’s available with packages and other assistance that help.
Furthermore, your treatment will perform by the top experienced fertility experts. They use their top education and information in performing successful treatments. With it, you will get many benefits and facilities for the best process.
History of PGD in India – PGS
IVF was first successfully used in 1978. This was not until years later that scientists started fiddling with the option for taking out one or more cells from the embryo to get information about the possible health of the child that might result following implantation of that embryo.
The first report of pre-implantation genetic testing in humans with a pregnancy resulting went published in 1990. Major developments in these technologies have been expanded since then. Both the embryo biopsy techniques with the genetics technologies employed on cells removed from embryos have enhanced noticeably.
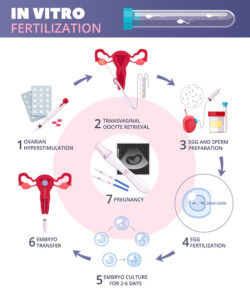
How is IVF-PGS performed?
At us, the initial part of the IVF cycle is performed in the same way as for infertility and gets made of five basic steps:
- Developing of the eggs;
- Recovery of the eggs;
- Fertilization of the eggs and expansion of the resultant embryos;
- Biopsy of the embryos and CGH to display the embryos for chromosomal abnormalities;
- Freezing of the embryos to obtain the test results and moving unchanged embryos in a frozen embryo cycle (FET).
IVF Treatment Success Rates in India
IVF success rate in India is much higher which helps achieve successful outcomes. You can have the best outcome by managing the conditions. Still, your success rate of IVF in India depends on various factors.Your IVF success rates will be as per your age. Such as:
for women under age 30
for women age 35 - 37
for women ages 38 - 40
for women over age 41
The couple’s age, infertility conditions, centre you choose health status, and other aspects. These are highly responsible for affecting your IVF treatment. Your IVF success rates in India depend on various factors, such as:
- Moreover, you can have advanced procedures and approaches for increasing the conception chances.
- Your best fertility centre can help with the best method and approaches.
- These depend on your infertility and health conditions. Your fertility expert will suggest they increase the treatment outcome.
- Alternative to IVF-PGS
- Who get benefitted from PGD?
- PGD / PGS - checking the chromosomes
- PGD stands to Inherited Genetic Diseases
- PGD comes to patients of chromosomal translocations
- Concerns with PGD
- When is PGD suggested?
- Patients that are having IVF with advanced females age – 38 or older (common)
- Patients of any age with repeated IVF failure – usually defined as 3 or more failed attempts
- To screen for inherited genetic diseases
- Patients that are carriers of chromosomal translocations
- Patients that have had recurrent miscarriages
- The main common reason that PGS is performed in the US is for “Advanced Age”.
- This would often indicate older than about 37 in many programs providing PGD in India.
- The logic recounts the fact that women of progressing age have enlarged rates of chromosomally irregular eggs – which after fertilization will turn into chromosomally abnormal embryos.
When the chromosomes in their sperm or eggs unite with those of their partner in the fertilized embryo, they have a towering percentage of chromosomal abnormalities. These embryos are at the very high risk for miscarriage or could cause to the birth of a child with birth defects. This is another situation where PGS could assist. By having IVF aneuploidy screening of the embryos, they could include chromosomally normal embryos transferred. Greatly this lessens their risk for miscarriage and birth defects.
- The embryos can be traumatized by the biopsy procedure, particularly for day 3 embryo biopsies
- There comes in vision that some evidence that cautiously executed trophectoderm biopsies done on day 5 and day 6 blastocysts might not fail the embryo at all
- As with any new technique and technology, there stands out a “learning curve”
- Some technicians will be more capable at the biopsy procedure
- Some genetics labs will be more talented at the analytical component after the cells get detached – providing a superior percentage of precise results
- As a result, there could be huge differences between centers executing these techniques, and even between technicians within the same IVF center
- Mosaicism can complicate matters. An embryo is a mosaic if there are 2 or more different chromosomal patterns in cells of that embryo
- There is evidence that mosaic embryos sometimes “self-repair”, or probably choose irregular cells preferentially to the placenta in place of the fetus. More research on mosaicism gets desirable
- X-chromosome-linked disorders like muscular dystrophies, Rhett syndrome, and hundreds of others that should be registered by a genetic counselor at a reproductive clinic.
- Single gene defects like cystic fibrosis, Tay-Sachs disease, sickle-cell anemia, and Huntington’s disease.
- Frequent miscarriages.
PGD Methods of Genetic Analysis
Normally SNPs happen all through a person’s DNA. They occur once in every 300 nucleotides on average, which stands that there are roughly 10 million SNPs in the human genome. Most commonly, these variations are found in the DNA between genes. They can act as biological markers, facilitating scientists put genes that are associated with disease. When SNPs take place within a gene or in a regulatory region near a gene, they could cooperate a more direct role in disease by affecting the gene’s function.
IVF Treatment with PGD
Why choose us: You can choose the best IVF centre in India for a successful outcome. We understand that couples face problems while deciding upon the treatment and place. But do not worry anymore because we are available with top-notch procedures and methods. Your infertility condition can have the best treatment accordingly. What else you will get through us?
Disclaimer, Gender Selection is Illegal in india and Not Done in India
Frequently Asked Questions About IVF Cost in India
Is India good for IVF?
The success rates of IVF in India are comparable with success rates in some of the biggest centers in the United States and Europe with pregnancy rates ranging between 50% to 60%.
What is the price of IVF in India?
The total cost of a basic IVF procedure in India is around USD 6,500 for one fresh cycle, however, if you undergo an advanced IVF procedure then the cost of IVF treatment in India will vary from USD 5,000 to USD 40,000 depending upon the advanced procedure of IVF you choose to treat the cause of infertility.
Is PGD available in India?
PGS treatment in India is common & widely available. PGD in India is becoming quite popular with couples who want to rule out genetic abnormalities.
Read Also:-

 WhatsApp us
WhatsApp us